Medical Implants and Metal Sensitivity: Balancing Biocompatibility, Durability, and Costs
The choice of material in medical implants today requires careful evaluation of the trade-offs between durability, biocompatibility, and the need for secondary interventions.
In the current landscape of reconstructive surgery, the selection of material for medical implants represents a complex clinical decision that balances multiple factors: from the patient's biological response to long-term healthcare costs. While permanent metals like titanium have dominated for decades, the emergence of bioresorbable materials and advanced polymers like PEEK is redefining the options available to surgeons and patients.
Bioresorbable Materials vs Permanent Metals: Comparative Analysis
The comparison between bioresorbable materials and permanent metals highlights different clinical and economic advantages, with significant impacts on the need for secondary interventions and the patient's inflammatory response.
Bioresorbable materials, particularly magnesium alloys, offer temporary mechanical support that gradually dissolves after the critical healing phase. This characteristic eliminates the need for secondary surgical interventions to remove the implant, reducing both patient risks and overall treatment costs. OsseoLabs has developed implants in bioresorbable magnesium that provide structural support during the bone healing phase, then resorb completely, avoiding the permanent presence of foreign hardware.
In contrast, permanent titanium implants guarantee long-term mechanical stability and have demonstrated excellent biocompatibility over decades of clinical use. However, they can cause complications related to the permanent presence of metal, including inflammatory reactions to wear debris and adaptation problems due to material rigidity. The “fundamental discrepancy” between standardized implants and the unique anatomy of each patient can lead to suboptimal load distribution and implant migration.
PEEK (polyether-ether-ketone) represents a third way: this high-performance polymer offers radiolucency, allowing post-operative imaging without artifacts, and an elastic modulus closer to that of bone than titanium, reducing stress shielding. Materialise has recently integrated PEEK into its portfolio of cranio-maxillo-facial implants, offering surgeons the freedom to choose between titanium and PEEK based on the specific needs of the clinical case.
Bone Integration and Advanced Structures: The Role of TPMS
TPMS surfaces significantly improve osseointegration but require advanced additive production technologies and rigorous quality controls, increasing complexity and initial costs.
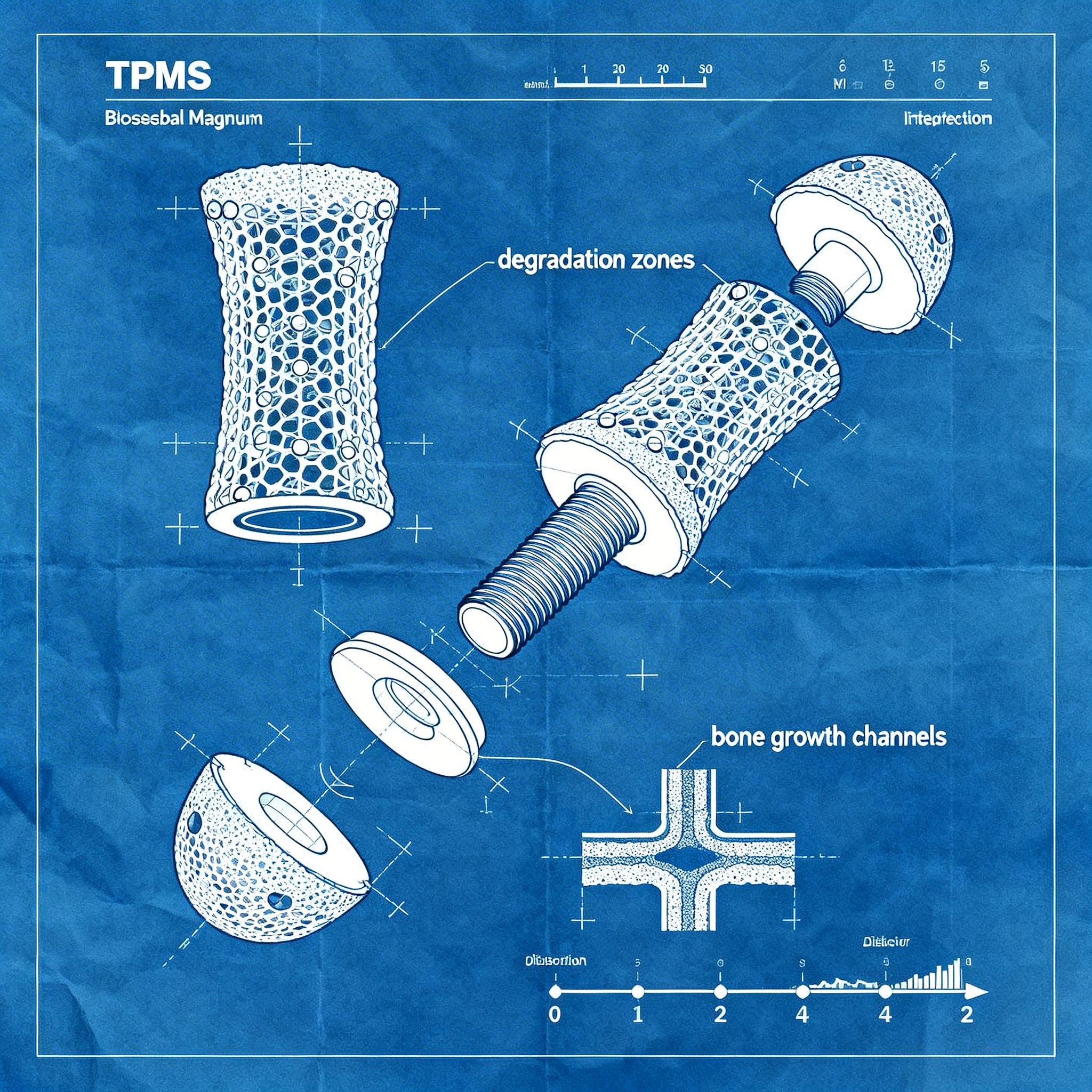
TPMS structures (Triply Periodic Minimal Surfaces) represent a significant innovation in implant engineering. The OsseoMatrix™ TPMS architecture developed by OsseoLabs promotes superior bone integration by creating a porous structure that facilitates bone tissue growth inside the implant. These complex geometries also reduce stress shielding, a phenomenon where an overly rigid implant prevents surrounding bone tissue from receiving adequate mechanical stimuli, causing it to weaken.
The production of TPMS structures in bioresorbible magnesium presents considerable technical challenges. Magnesium has a low melting point, high reactivity, and sensitivity to process instability, making additive printing particularly complex. OsseoLabs has invested significantly in the development of AI-driven design rules, topological optimization, and tightly controlled additive manufacturing processes, including proprietary laser pulsation techniques and degradation modeling.
Implants with hollow regions can be filled with bone grafts to further accelerate fusion and bone growth. Pilot clinical studies in dentistry and maxillofacial surgery show good integration, volumetric bone increase, and a reduction in the number of necessary interventions compared to traditional techniques with metal meshes.
Personalization and AI: Reducing Errors and Operating Times
Artificial intelligence and custom manufacturing transform surgical planning, reducing operating times by 30-50% in complex cases, but introducing greater design complexity and higher initial costs.
The OsseoVision™ platform uses artificial intelligence to complete segmentation and 3D anatomical reconstruction within one hour of uploading the high-resolution CT scan. Surgical planning and device design typically require 1-2 days, during which the system automates much of the implant and guide generation, including fixation strategy, topological optimization, and porous structure integration.
For surgeons, the main advantage is pre-operative confidence: they can digitally plan the procedure, review fixation strategies, and confirm implant positioning before entering the operating room. This reduces trial and error during the intervention, decreases intraoperative adjustments, and shortens surgical times often by 30-50% in complex cases. It also reduces cognitive load, which is particularly important in reconstructions where small decisions can have major downstream effects.
The digital workflow integrates design, simulations, production, and documentation under ISO 13485 certified systems. Polymer guides can be delivered within 24-48 hours, while metallic implants in titanium or bioresorbible magnesium typically require 3-7 days for printing, post-processing, and quality control. Materialise produces approximately 280,000 custom 3D-printed tools and implants per year, with partners like Ad Mirabiles guaranteeing production of PEEK implants within 72 hours of surgical plan approval.
Long-term Costs and Real Clinical Impact
Economic analysis of custom implants must consider not only higher initial costs, but also savings derived from fewer revisions, reduced operating times, and accelerated patient recovery.
At the healthcare system level, the benefits of customization and advanced materials translate into concrete economic advantages. Faster planning, shorter procedures, fewer complications, and a reduction in revision or removal surgeries lead to lower total costs per case. For payment systems and public healthcare, this is not just about economic savings, but the possibility of making advanced reconstructive care scalable and accessible.
Bioresorbable implants completely eliminate the need for secondary removal procedures, with savings estimated at thousands of euros per patient and a reduction in risks associated with further surgical procedures. Faster recovery allows patients to return to daily activities sooner, with indirect socioeconomic benefits.
However, the initial costs of customized implants and advanced technologies are significantly higher than those of standardized implants. The production of TPMS structures in magnesium, with rigorous quality controls and proprietary processes, requires considerable technological investment. The regulatory complexity of customized devices, which sit at the intersection of customization and compliance, adds further costs for documentation and risk management.
The choice between PEEK and titanium also involves economic considerations: PEEK requires closed and heated chamber printing systems, high-temperature plans, and accurate thermal profile management to control the polymer's crystallinity. These specific technical requirements can influence production costs and delivery times.
Conclusion
The selection of the ideal material for a medical implant requires a multidimensional evaluation that takes into account safety, efficacy, and economic sustainability, balancing immediate clinical benefits with long-term outcomes.
The future of medical implants does not lie in the supremacy of a single material, but in the ability to select the optimal solution for each specific case. Bioresorbable materials offer significant clinical and economic advantages by eliminating secondary interventions, while PEEK and titanium maintain important roles.
article written with the help of artificial intelligence systems
Q&A
- What are the main advantages of bioresorbable materials compared to permanent metals in medical implants?
- Bioresorbable materials, such as magnesium alloys, offer temporary mechanical support that dissolves after healing, eliminating the need for secondary removal procedures. This reduces risks for the patient and the overall costs of treatment.
- How does PEEK differ from titanium in medical implants?
- PEEK is a polymer with radiolucency that allows for post-operative imaging without artifacts and has an elastic modulus more similar to that of bone, reducing stress shielding. Titanium, on the other hand, guarantees long-term mechanical stability but can cause inflammatory reactions and anatomical adaptation problems.
- What are TPMS structures and what is their role in medical implants?
- TPMS (Triply Periodic Minimal Surfaces) structures are porous architectures that improve osseointegration by promoting bone tissue growth inside the implant. They also reduce stress shielding and require advanced production technologies such as 3D printing.
- How does artificial intelligence contribute to the personalization of medical implants?
- Artificial intelligence accelerates surgical planning by automating segmentation and 3D reconstruction, reducing operating times by 30-50%. It also enables topological optimization and the design of custom implants, improving precision and clinical outcomes.
- What are the main economic disadvantages of custom implants compared to standardized ones?
- Custom implants have higher initial costs due to design complexity, additive production, and required quality controls. In addition, specific regulation for custom devices increases documentation and risk management costs.