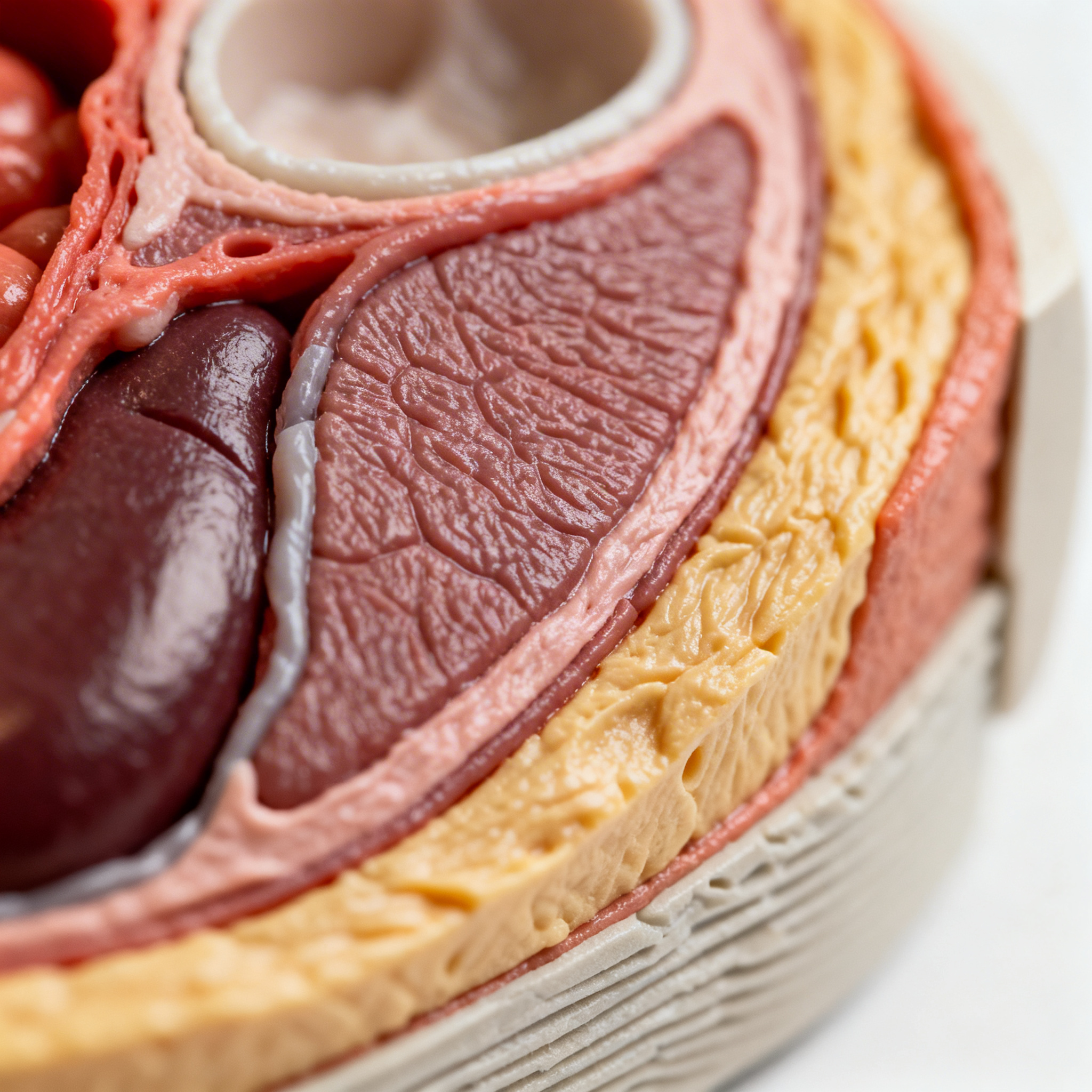
How 3D Anatomical Models Work in Surgical Planning for Medical Education
A 3D-printed facial model is revolutionizing surgeon training, allowing simulated interventions on artificial but realistically stratified tissues. Thanks to the combination of advanced materials and multi-layer printing technologies, 3D anatomical models allow future healthcare professionals to practice on complex procedures without risk to patients, accurately reproducing the physical properties of human tissues.
Anatomical Design of 3D Models
3D anatomical models originate from the transformation of radiological data into replicas faithful to clinical reality, enabling accurate and personalized surgical planning.
The process of creating anatomical models for surgical training begins with the acquisition of high-resolution images via CT or CBCT (Cone Beam Computed Tomography). This data is processed through specialized software that performs automatic segmentation of anatomical structures, completing an accurate 3D reconstruction in approximately one hour. AI-driven technology allows for the identification and separation of different anatomical components – bones, muscles, nerves, blood vessels – creating a complete digital map of the region to be replicated.
In the case of facial models developed by Addion GmbH in collaboration with the University of Innsbruck, anatomical design focuses on the ocular and periorbital region, replicating complex structures such as the orbicularis muscle, orbital septum, upper tarsal plate, ligaments, and facial nerve. Each element is colored distinctively in the final model, facilitating identification by training surgeons and allowing them to understand which structures can be manipulated and which must be preserved during the intervention.
Multi-layer Materials for Tissue Simulation
Multi-material 3D printing technologies allow for the replication of the mechanical and tactile properties of human tissues through precise combinations of specialized materials.
The most advanced anatomical models use up to eight different materials to faithfully reproduce the characteristics of human tissues. Stratasys' PolyJet technology, employed in the Digital Anatomy Solution, allows for combining materials with different hardnesses, transparencies, flexibilities, and resistances within the same model. Each layer is designed to respond predictably during dissection: skin presents the correct resistance to cutting and maintains connection with the underlying tissue, muscles show appropriate consistency, while blood vessels release a red liquid that simulates bleeding when incised.
The anatomical presets developed by Stratasys for dental and medical applications use predefined parameters that control how materials are mixed and distributed within the model, using specific ratios and patterns to achieve consistent and repeatable results. This standardization allows medical institutions to produce musculoskeletal and anatomical systems that biomechanically and accurately reproduce real human anatomy, while maintaining the possibility of customization based on CBCT scan data to reflect specific patient pathologies.
Model Construction and Calibration Process
From initial scanning to final printing, the production process involves precise phases of validation and quality control to ensure anatomical and functional accuracy.
Once digital design is complete, the physical production of the model follows a strictly controlled workflow. Polymer surgical guides can be delivered within 24-48 hours, while metal implants and complex anatomical models typically require 3-7 days for printing, post-processing, and quality assurance. All devices undergo dimensional checks and validation according to ISO 13485 workflows, ensuring that each model meets the required quality standards for educational and clinical use.
For reusable models for medical education, such as the one developed at Iowa State University for meniscal injuries, the process involves 3D printing of rigid bone components and creating molds for flexible parts. Plastisol, a flexible plastic material, is heated to a fluid state, cast into 3D printed molds, and allowed to solidify to obtain inserts that can be mounted on bone structures. This feature allows the material to be cut, heated, and reformed multiple times, enabling students to practice on multiple injury scenarios with the same set of components.
Didactic Applications in Surgical Training Courses
3D models are used to teach complex surgical techniques, allowing students to connect anatomical theory with clinical practice in a safe and effective manner.
By November 2025, 40 surgeons in training at the Anatomical Institute of the University of Innsbruck have used 3D printed facial models to practice on ocular and periorbital procedures. During training sessions, students perform realistic incisions, separate skin layers from underlying muscle tissue, identify critical structures such as the facial nerve (which must not be damaged), and practice complete sutures. According to Alexander Hechenberger, CEO of Addion, “for almost every ocular pathology there is a specific model,” making medical education more accessible and practical compared to traditional methods based on body or animal donors.
In the dental sector, Stratasys anatomical presets are used in classrooms and clinics to practice surgical techniques such as tooth extractions, implant placement, periodontal surgery, endodontic surgery, and sinus augmentation. Medical and dental device manufacturers can also use these models to accelerate clinical adoption through high-quality practical demonstrations and to shorten development cycles by testing tools and techniques on anatomically accurate replicas.
Student Feedback and Evaluation of Educational Effectiveness
Studies and testimonials demonstrate that 3D models significantly improve anatomical understanding and practical preparation of future surgeons.
Student testimonials highlight how traditional manuals can only go so far in understanding dynamic anatomy. As reported by students from Iowa State University, “not being able to take someone's leg off to see the inside of the knee,” having a model in front of them that shows the meniscus in motion helps to understand how different stresses generate injuries and why some symptoms appear, disappear, or remain silent. Directors of Athletic Training programs emphasize the importance of having teaching tools that allow students not only to memorize definitions, but to actually demonstrate what is being talked about when describing a specific injury to a patient.
The models allow for connecting the “mechanism” of the injury – the dynamics of the movement that causes the damage – with the observed clinical “result” in the form of rupture patterns, pain, joint locking, or instability. This more intuitive mechanical understanding better prepares students to communicate with patients and make informed decisions based on solid practical knowledge, bringing learning to a new level compared to traditional teaching methods.
Conclusion
3D anatomical models represent an increasingly essential tool for safe and effective medical education. The ability to faithfully replicate the physical properties of human tissues through multi-layer materials, combined with the possibility of customization based on real radiological data, offers surgical trainees unprecedented hands-on experience. The integration between 3D imaging, digital modeling, and advanced printing allows for “putting in hand” complex anatomy before operating on real patients, significantly reducing risks and improving professional preparation.
Educational institutions should invest in advanced simulation technologies to best prepare future healthcare professionals. With the continuous evolution of materials and 3D printing techniques, these teaching tools will become increasingly accessible and indispensable for ensuring high standards in training.
article written with the help of artificial intelligence systems
Q&A
- What is the main advantage of 3D anatomical models in medical education?
- 3D anatomical models allow future surgeons to practice complex procedures safely, without risks to patients. They faithfully replicate the physical properties of human tissues, allowing for realistic and personalized training.
- How are 3D anatomical models created for surgical training?
- The models are obtained by transforming radiological data, such as CT or CBCT, into accurate replicas of clinical reality. Through specialized software and AI-driven technologies, automatic segmentation of anatomical structures is performed to create a precise 3D reconstruction.
- What materials are used to make the models realistic?
- Multimaterial 3D printing technologies, such as Stratasys PolyJet, use up to eight different materials to replicate the mechanical and tactile properties of human tissues. These include materials with different hardnesses, transparencies, and flexibilities to simulate skin, muscles, and blood vessels.
- How are 3D models used in surgical training courses?
- Models are used to teach complex surgical techniques, allowing students to practice on incisions, sutures, and the identification of critical structures such as the facial nerve. They are also used to simulate specific pathologies and improve practical understanding of anatomy.
- What is the importance of student feedback on the use of 3D models?
- Students report that 3D models offer a deeper and more practical understanding of anatomy compared to traditional manuals. They allow for the visualization and manipulation of internal structures in motion, improving learning and the ability to communicate with patients.